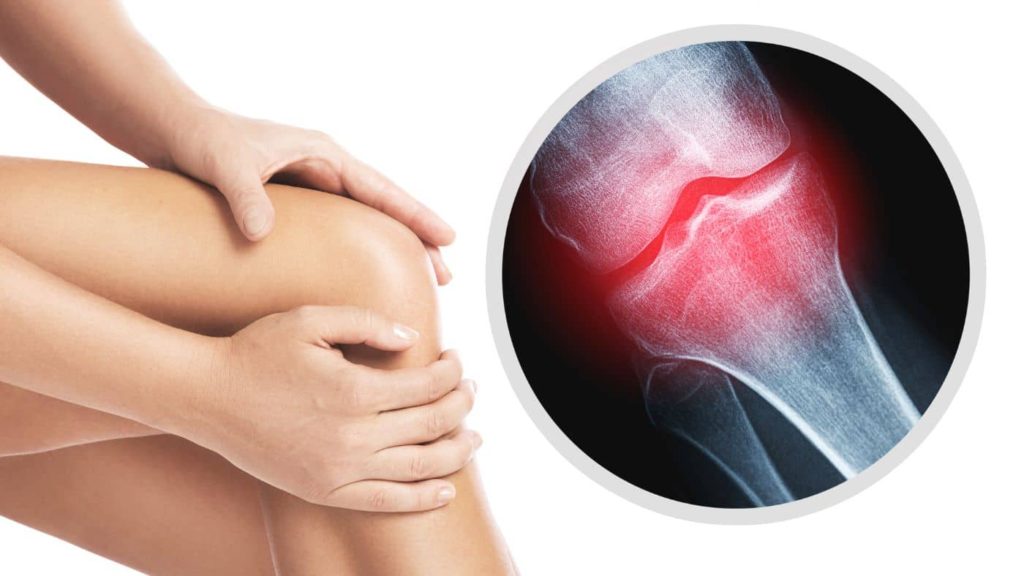
Osteoarthritis, a common degenerative joint disease, poses a significant challenge to millions of people worldwide. While the condition can often feel overwhelming, taking the time to understand its symptoms, diagnosis, treatment, and prevention can empower individuals to manage their condition effectively. This comprehensive guide will explore how osteoarthritis affects the body, discuss risk factors, and provide valuable insights into prevention and management strategies to help individuals live their best lives.
Key Takeaways
Osteoarthritis is a chronic joint condition causing pain, stiffness and reduced mobility.
Effective management of osteoarthritis involves lifestyle modifications, medications/injections or surgery, physical therapy, and assistive devices.
Support groups and resources are available to help individuals living with osteoarthritis maintain independence & quality of life.
Understanding Osteoarthritis
Osteoarthritis is a degenerative joint disease that affects a multitude of people, causing pain, stiffness, and reduced mobility. As the most common form of arthritis, it is vital to understand the nature of the condition, how it affects joints, and which joints are commonly affected.
We now delve into the intricacies of osteoarthritis and explore its impact on the body.
What is Osteoarthritis?
Osteoarthritis is a chronic condition characterized by the deterioration of joint cartilage, leading to pain and stiffness. There are two types of osteoarthritis: primary and secondary. Primary osteoarthritis has no identifiable cause, while secondary osteoarthritis results from another disease, infection, joint injury, or deformity.
The condition is a common form of arthritis, and bone spurs, or bony outgrowths, often manifest in those affected. Fluid-filled cysts may also develop, limiting joint movement and causing discomfort.
How Osteoarthritis Affects Joints
Osteoarthritis affects joints by causing cartilage breakdown, bone spurs, and inflammation. These factors contribute to joint pain, stiffness, and decreased mobility. The spine, for instance, can be affected by osteoarthritis, leading to narrowed disks and bone spur formation.
The synovial membrane, which serves as a cushion of fluid that lubricates joints, also reduces symptoms. Tendons and ligaments provide support to joints, with pain relievers available to alleviate discomfort caused by osteoarthritis.
Commonly Affected Joints
Osteoarthritis can affect any joint in the body. It is more commonly found in the following areas:
Hands
Knees
Hips
Lower back
Neck
The condition primarily targets weight-bearing joints, such as the hip joint, knee, and spine, but other joints, like the hands and hips, may also be affected.
Knowing the joints commonly affected aids in taking preventive measures and seeking proper treatment when necessary.
Symptoms of Osteoarthritis
Early diagnosis and effective management of osteoarthritis hinge on recognition of its symptoms. The primary indicators of osteoarthritis are:
Joint pain
Joint stiffness (particularly after rest or inactivity)
Decreased range of motion in the joint over time
A grating sensation of the joint when moved
This section presents a discussion on various osteoarthritis symptoms and their impact on daily life.
Pain and Stiffness
Joint pain and stiffness are the primary symptoms of osteoarthritis, often experienced in affected joints during or after activities such as walking, running, or climbing stairs.
Interestingly, rest or changing positions, such as sitting or lying down, can help alleviate pain and stiffness. Balancing activity and rest is a key strategy in managing these symptoms and retaining overall joint health.
Reduced Range of Motion
Another common symptom of osteoarthritis is a reduced range of motion in affected joints. This limitation in movement can make it difficult to perform daily tasks and hinder overall mobility.
Joint stiffness and muscle weakness may be particularly noticeable after periods of inactivity, such as when first awakening or during and after movement. Addressing these symptoms is necessary to limit joint movement and preserve independence and quality of life.
Other Symptoms
In addition to pain, stiffness, and reduced range of motion, osteoarthritis may present with other symptoms, such as joint swelling, tenderness, and a grating sensation when the joint is in motion. Inflammation of the joint, damage to cartilage, and the formation of bone spurs may be the underlying causes of these symptoms.
Lifestyle modifications, medications, and physical therapy can be employed to reduce symptoms, manage these additional symptoms, and further improve quality of life.
Risk Factors for Osteoarthritis
Understanding the risk factors associated with osteoarthritis can help individuals take preventive measures and seek appropriate treatment when necessary. Some of the primary risk factors include:
Age
Genetics
Weight
Joint injuries
This section delves into a detailed discussion on these risk factors and their role in osteoarthritis development.
Age and Genetics
Age and genetics play significant roles in the development of osteoarthritis. As individuals age, the risk of developing the condition increases. Genetics can also contribute to the development of osteoarthritis, as certain genetic mutations can increase the likelihood of developing the condition, and those with a family history of osteoarthritis are more likely to be affected.
Appreciating how age and genetics contribute to osteoarthritis can guide individuals in taking appropriate preventive measures.
Weight and Joint Injuries
Excess weight and joint injuries can increase the risk of developing osteoarthritis by placing additional stress on joints. It has been found that being overweight or obese increases the risk of osteoarthritis, with overweight women having nearly four times the risk of knee osteoarthritis and overweight men having five times the risk.
Joint injuries can also heighten the risk of developing osteoarthritis, as injury to the joint can damage cartilage, causing inflammation and pain, which can lead to further joint damage and an increased risk of the condition.
Additional Risk Factors
Additional risk factors for osteoarthritis include:
Gender: Women are more susceptible to developing osteoarthritis than men.
Occupation: Certain occupations, such as manual labor, may be associated with a heightened risk of the condition.
Medical conditions: Certain medical conditions, such as obesity and diabetes, can increase the risk of developing osteoarthritis.
Medical conditions, such as diabetes, gout, and rheumatoid arthritis, have been linked to an elevated risk of osteoarthritis. Being aware of these additional risk factors can help individuals take preventive measures and seek appropriate treatment when necessary.
Diagnosing Osteoarthritis
Diagnosing osteoarthritis involves the following steps:
Obtaining a patient’s medical history
Performing a physical examination
Conducting imaging exams
Running blood tests
These steps are essential in obtaining appropriate treatment and managing the condition effectively.
This segment discusses the different facets of the diagnostic process and their significance in osteoarthritis identification and treatment.
Medical History and Physical Examination
Medical history and physical examination are two essential components of diagnosing osteoarthritis. Gathering a comprehensive medical history of the patient’s symptoms, lifestyle, and medical history is crucial. Additionally, a physical examination of the affected joints to assess for signs of osteoarthritis is also necessary.
Healthcare providers may use this information to rule out other potential causes of symptoms and determine the most appropriate course of treatment.
Imaging Exams
Imaging exams, such as X-rays, MRI, and ultrasound, play a vital role in the diagnosis of osteoarthritis. These imaging techniques can help visualize joint damage and confirm an osteoarthritis diagnosis.
In some cases, imaging exams may also be utilized to monitor the progression of the condition and assess the effectiveness of treatment.
Blood Tests
Although there are no specific blood tests used to diagnose osteoarthritis, blood tests can help rule out other conditions and detect markers of inflammation or gout.
By identifying other potential causes of joint pain and soft tissue inflammation, healthcare providers can ensure that patients receive the most appropriate treatment for their specific condition.
Treatment Options for Osteoarthritis

Once diagnosed, it is essential to explore the various treatment options available for managing osteoarthritis. These options may include:
Conservative treatments
Medications
Injections
Surgery
We delve into these treatment options in this section, providing insights on how they can enhance the quality of life for those living with osteoarthritis.
Conservative Treatments
Conservative treatments for osteoarthritis include modifications to lifestyle, physical therapy, and the application of heat or cold therapy.
Lifestyle changes, such as maintaining a healthy weight and consuming a balanced diet, can help prevent and manage osteoarthritis. Physical therapy can also be beneficial, as it can help strengthen the muscles around the affected joint, improve range of motion, and reduce pain. Heat or cold therapy can further help alleviate pain and inflammation.
Medications and Injections
Medications and injections can help manage pain and inflammation associated with osteoarthritis. Nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, and hyaluronic acid injections are commonly employed to manage the condition.
While these medications can alleviate pain and reduce inflammation, consultation with a healthcare provider to discuss potential risks, benefits, and side effects is necessary.
Surgical Options
For severe cases of osteoarthritis, joint surgery may be considered when conservative treatments have been ineffective. Surgical interventions can include joint replacement, joint fusion, and osteotomy.
Surgery can help relieve pain and improve mobility, but it is important to weigh the potential risks and benefits of these procedures and consult with a healthcare provider before pursuing surgical intervention.
How an Osteopath Can Help

Osteopaths can play a vital role in managing osteoarthritis through hands-on treatments and a holistic approach to patient care. Osteopathic medicine has a long history of treating musculoskeletal conditions, such as osteoarthritis.
This section delves into the history of osteopathic medicine and the role of osteopaths in aiding individuals with osteoarthritis through various treatments.
History of Osteopathic Medicine
Osteopathic medicine has its roots in the 19th century when Dr. Andrew Taylor Still established the practice in 1874. Since then, osteopathic medicine has grown in recognition, with the first osteopathic medical school established in 1892. Today, there are more than 102,000 osteopathic medical doctors in the United States.
Osteopathic medicine’s long-standing focus on treating musculoskeletal conditions makes it a valuable resource for individuals with osteoarthritis.
Osteopathic treatments for Osteoarthritis
One of the key treatments in osteopathic medicine is osteopathic manipulative therapy (OMT), a hands-on treatment that can help improve joint function and reduce pain in osteoarthritis patients. Osteopaths use a holistic approach to patient care, treating the body, mind, and spirit as an interconnected system.
By addressing the root cause of symptoms and providing targeted treatments like OMT, osteopaths can help ameliorate symptoms and increase overall quality of life for those living with osteoarthritis.
Preventing and Managing Osteoarthritis
Preventing and managing osteoarthritis involves making lifestyle changes, maintaining a healthy weight, and engaging in regular exercise and physical therapy.
Various strategies and interventions useful in preventing and managing osteoarthritis, thereby ensuring better quality of life and overall well-being, are discussed in this section.
Lifestyle Changes

Implementing lifestyle changes can be a powerful tool in preventing and managing osteoarthritis. Consuming a balanced diet, abstaining from smoking, and drinking alcohol in moderation can help support overall health and reduce the risk of developing osteoarthritis.
Stress management, including practicing relaxation techniques and engaging in activities that promote mental well-being, can also contribute to preventing and managing the condition.
Maintaining a Healthy Weight
Maintaining a healthy weight is crucial in preventing the development or progression of osteoarthritis. Excessive weight places additional stress on joints, increasing the likelihood of developing the condition and exacerbating existing symptoms.
Consuming a balanced diet and engaging in regular exercise can help individuals maintain a healthy weight and reduce the strain on their joints.
Exercise and Physical Therapy
Exercise and physical therapy play a critical role in preventing and managing osteoarthritis. Regular, low-impact activities such as walking, swimming, and cycling can help maintain joint flexibility and strength.
Strength training and stretching exercises can also be beneficial for individuals with osteoarthritis. Physical therapists can provide guidance on how to safely perform exercises and activities to manage the condition.
Living with Osteoarthritis
Living with osteoarthritis can pose challenges and require adaptations in daily life. However, with the right support and resources, individuals can manage their condition effectively and maintain their independence.
This section discusses strategies for daily task management, seeking support and resources, and using assistive devices to help individuals live well with osteoarthritis.
Daily Task Management

Managing daily tasks with osteoarthritis involves pacing activities, using proper body mechanics, and modifying tasks to reduce joint stress. For example, it is important to distribute activities throughout the day, allowing for rest periods between.
Using proper body mechanics, such as lifting with the legs rather than the back, can also help protect joints and reduce pain. Modifying tasks, such as using a cart to carry groceries, can further reduce joint stress and help manage osteoarthritis symptoms.
Support and Resources
Support and resources are invaluable for individuals living with osteoarthritis. Support groups, such as the Arthritis Foundation and the Osteoarthritis Support Group, offer an opportunity to connect with others facing similar challenges and share experiences and advice.
Educational materials, such as books, pamphlets, and online resources, can also provide valuable information about the condition, its symptoms, and treatment options.
Assistive Devices
Assistive devices, such as canes, walkers, and braces, can help improve mobility and reduce pain for those living with osteoarthritis. These devices can provide additional support and stability, reducing the strain on affected joints.
It is important to consult with a healthcare professional when selecting assistive devices to ensure proper fit and function.
Summary
In conclusion, osteoarthritis is a widespread degenerative joint disease that affects millions of people worldwide. By understanding its symptoms, risk factors, diagnosis, and treatment options, individuals can effectively manage their condition and maintain their quality of life. Embracing lifestyle changes, seeking appropriate medical care, and utilizing support and resources can make a significant difference in the lives of those living with osteoarthritis. Remember, you are not alone in your journey, and with the right tools and strategies, you can thrive despite the challenges posed by this condition.
Frequently Asked Questions
What is the best treatment of osteoarthritis?
The best treatment for osteoarthritis is to maintain a healthy weight, exercise regularly, take medication to relieve pain, and use supportive therapies to make everyday activities easier.
What are the 4 signs of osteoarthritis?
Osteoarthritis symptoms include swelling and tenderness, stiffness after getting out of bed, a crunching feeling or sound of bone rubbing on bone, as well as pain in hands, lower back, neck, and weight-bearing joints such as knees, hips, and feet.
Pain can be felt in the hands, lower back, neck, and weight-bearing joints such as knees, hips, and feet. Swelling and tenderness are common symptoms, as well as a crunching feeling or sound of bone rubbing on bone. Stiffness after getting out of bed is also a symptom of osteoarthritis.
What is the main cause of osteoarthritis?
Osteoarthritis is caused by the breakdown of cartilage in the joint, leading to thickening and bony growths.
Secondary osteoarthritis can be caused by other factors such as disease, infection, injury, or deformity.
What’s the difference between arthritis and osteoarthritis?
Osteoarthritis is a type of arthritis caused by mechanical wear and tear on joints, whereas rheumatoid arthritis is an autoimmune disease in which the body’s immune system attacks the joints.
Osteoarthritis is the most common form of arthritis and involves the wearing away of cartilage that caps the bones in your joints.
What is the difference between primary and secondary osteoarthritis?
Primary osteoarthritis has no identifiable cause, whereas secondary osteoarthritis is caused by an outside factor, such as another disease, infection, joint injury, or deformity.
These outside factors can lead to the breakdown of cartilage, which is the cushion between bones in a joint. This breakdown can cause pain, swelling, and stiffness in the joint.